- Wine and health — why is there so much argument, pro and con?
- Why we are never going to know whether wine is good for us, or not
- Health and the wine drinker, yet again
- Wine and health is never a simple topic
However, I thought that in my post I might write about the most comprehensive scientific study ever undertaken involving alcohol effects. This sort of study is called a meta-analysis, and it tries to combine all of the data from all of the known published studies into one giant dataset, and then see what general conclusions might be drawn.
For medicine, this approach is taken globally by what is called the Global Burden of Disease Study. As they themselves claim:
The Global Burden of Disease (GBD) provides a comprehensive picture of mortality and disability across countries, time, age, and sex. It quantifies health loss from hundreds of diseases, injuries, and risk factors, so that health systems can be improved and disparities eliminated.The GBD has been going for the past three decades (The Global Burden of Disease Study at 30 years), and it has become more and more ambitious:
The Global Burden of Disease Study (GBD) began 30 years ago with the goal of providing timely, valid and relevant assessments of critical health outcomes ... The latest iteration provides assessments of thousands of outcomes for diseases, injuries and risk factors in more than 200 countries and territories and at the subnational level in more than 20 countries. The GBD is now produced by an active collaboration of over 8,000 scientists and analysts from more than 150 countries.For our purposes here, the most recent publication looking at the effects of alcohol appeared back in 2016:
Alcohol use and burden for 195 countries and territories, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016.
There are 514 authors who contributed to the publication, based on “694 data sources of individual and population-level alcohol consumption, along with 592 prospective and retrospective studies on the risk of alcohol use” (you should be very very impressed by this!). From all of this, they “produced estimates of the prevalence of current drinking, abstention, the distribution of alcohol consumption among current drinkers in standard drinks daily (defined as 10 g of pure ethyl alcohol), and alcohol–attributable deaths and DALYs [disability-adjusted life-years]”.
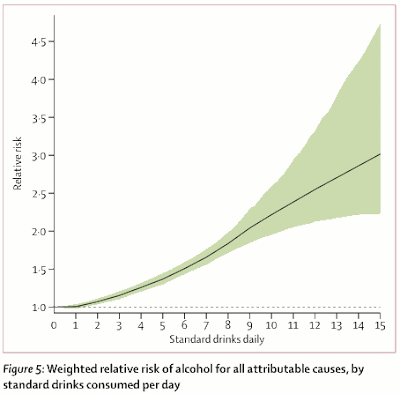
You can read the paper for yourself if you want the details, but the conclusions are clear (see the graph above):
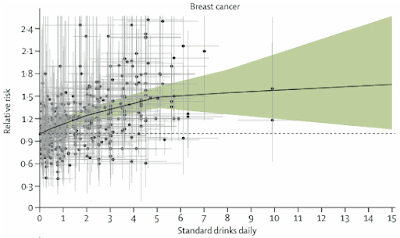
Alcohol use is a leading risk factor for global disease burden and causes substantial health loss. We found that the risk of all-cause mortality, and of cancers specifically, rises with increasing levels of consumption, and the level of consumption that minimises health loss is zero ... Globally, alcohol use was the seventh leading risk factor for both deaths and DALYs in 2016, accounting for 2.2% of age–standardised female deaths and 6.8% of age–standardised male deaths.There are lists of different medical conditions associated with increasing alcohol consumption — one of these, which you may not have thought of, is illustrated in the graph below. Nevertheless, the bottom line is clear:
The level of alcohol consumption that minimised harm across health outcomes was zero standard drinks per week.
Now, you might not like this conclusion, especially as it does seem to contradict those studies reporting apparently protective effects of small amounts of alcohol consumption. Indeed, a more recent meta-analysis (2023) does report such a thing (Association between daily alcohol intake and risk of all-cause mortality: A systematic review and meta-analyses):
This systematic review and meta–analysis of 107 cohort studies involving more than 4.8 million participants found no significant reductions in risk of all-cause mortality for drinkers who drank less than 25 g of ethanol per day (about 2 standard drinks compared with lifetime nondrinkers) after adjustment for key study characteristics such as median age and sex of study cohorts.That is, less than 2 drinks per day did not increase health risks. So, I guess this contradiction means that we still don’t know anything consistent about small alcohol effects, and maybe we never will.*
* The issue here seems to be that combining data from different studies has all sorts of technical (data–analysis) issues arising from different biases in the original data:
Mounting evidence suggests these associations might be due to systematic biases that affect many studies. For example, light and moderate drinkers are systematically healthier than current abstainers on a range of health indicators unlikely to be associated with alcohol use — eg, dental hygiene, exercise routines, diet, weight, income; lifetime abstainers may be systematically biased toward poorer health; studies fail to control for biases in the abstainer reference group, in particular failing to remove “sick quitters” or former drinkers, many of whom cut down or stop for health reasons; and most studies have nonrepresentative samples leading to an over-representation of older White men.


This brief report on limited studies appears to reveal... nothing of substance?
ReplyDeleteOne thing I am confident all medical professionals will agree upon is that the regular consumption of alcohol will not make you "healthier". However, any in depth health study will uncover so many activities that have a negative impact on health, whether it be sedentary lifestyle, consumption of alcohol, sugar, fats, carbs, toxic chemicals, too much sun exposure, too little sun exposure the list will go on and on.
At this stage in our evolution, our mortality is inevitable. Once that is accepted, quality of live is the large variable. If moderate alcohol consumption significantly improves quality of life, that in itself has value and benefits.
As for the effects of alcohol on the body? If there is an article to be written on this topic, perhaps it would be useful to describe the tangible impacts of alcohol on the various organs of the human body at various levels of consumption, and determine positive or negative net response for the different components.
This is a brief summary, not a medical review article. Very few people would read the latter, I think.
ReplyDelete